Hantavirus Outbreak on Cruise Ship Sparks Public Concern, Recontextualizes Risk for Outdoor Enthusiasts
In recent weeks, an unusual outbreak of hantavirus aboard a cruise ship, which tragically claimed three lives, has led to a dramatic surge in public awareness and concern. Google searches for the rare disease have escalated by over 1,000% in some regions, reflecting a heightened global curiosity about a pathogen most people rarely encounter. While the virus is generally considered uncommon and challenging for the average individual to contract, this particular incident saw as many as 17 American passengers aboard the vessel reportedly infected. These passengers returned to the United States on Monday and are now under rigorous monitoring at the National Quarantine Unit located at the University of Nebraska Medical Center, a facility renowned for its biocontainment capabilities. This incident, while alarming, serves as a critical reminder that the primary demographic at elevated risk for hantavirus infection remains individuals, such as backpackers and others, who spend significant time in wooded or wilderness areas where contact with rodents is more probable. Adhering to a few key prevention strategies can substantially mitigate this inherent risk.
The Cruise Ship Incident: A Rare Transmission Event
The specifics of the hantavirus outbreak on the cruise ship are particularly noteworthy due to its unusual nature. While health officials have yet to definitively pinpoint the exact cause of the onboard transmission, preliminary findings suggest the strain involved was a rare variant originating from the Andes region. This specific strain, unlike the more common types found in North America, possesses the capability for human-to-human transmission, a factor that significantly complicated the management of the outbreak and necessitated stringent quarantine measures. This characteristic explains the heightened caution exercised during the repatriation of affected passengers, with some requiring transport in specialized biocontainment units, as reported by The New York Times. The sudden appearance of such a strain in an environment like a cruise ship, typically considered distinct from its natural reservoir, underscores the complexities of global health and disease vector management in an interconnected world.
The chronology of events began with initial reports of passengers falling ill during the cruise. As the severity of the illness became apparent and hantavirus was identified as the cause, health authorities initiated a rapid response. This involved identifying and isolating suspected cases, conducting contact tracing among passengers and crew, and coordinating with international health organizations. Upon the ship’s return to port, the 17 American passengers displaying symptoms or identified as close contacts were promptly transferred to the National Quarantine Unit. The decision to house them at the University of Nebraska Medical Center highlights its specialized expertise and infrastructure for managing highly infectious diseases, ensuring both patient care and the prevention of further community spread. The monitoring period for these individuals is crucial, given the variable incubation period of hantavirus, which can range from one to eight weeks.
Understanding Hantavirus: A Scientific Overview
Hantavirus is not a single pathogen but rather a general term encompassing several distinct viruses, each capable of causing severe, sometimes fatal, diseases in humans. According to the Centers for Disease Control and Prevention (CDC), these pathogens are responsible for two primary syndromes. The first, and most prevalent in the Western Hemisphere, is Hantavirus Pulmonary Syndrome (HPS). This condition is characterized by a two-phase illness. Initial symptoms, which can be non-specific and mimic common viral infections, typically include profound fatigue, fever, and muscle aches, often localized in the hips, back, and shoulders. These symptoms may persist for several days.
However, the disease progresses critically in the second phase, usually appearing four to ten days after the onset of initial symptoms. During this stage, the patient’s lungs begin to fill with fluid, leading to acute respiratory distress. Symptoms intensify, including a persistent cough and severe shortness of breath, reflecting the compromised pulmonary function. HPS is a life-threatening condition, carrying a significant fatality rate of approximately 38%, underscoring the urgency of early diagnosis and intensive medical care. Despite advances in supportive care, there is currently no specific antiviral treatment for hantavirus infection, and management primarily focuses on respiratory support and fluid management.
The second major type of hantavirus-related illness is Hemorrhagic Fever with Renal Syndrome (HFRS), which is predominantly observed in Europe and Asia. Unlike HPS, HFRS primarily targets the kidneys, leading to a different constellation of symptoms. Patients typically experience intense headaches, nausea, fever and chills, and blurred vision, alongside signs of renal dysfunction. While also serious, the fatality rate for HFRS is generally lower than HPS, ranging from 5% to 15%. Crucially, for both HPS and HFRS, there is currently no available vaccine, making prevention through avoiding exposure the cornerstone of public health efforts.

A close-up rendering of the hantavirus. Image: Shutterstock
Transmission Pathways and Primary Risk Factors
The vast majority of hantavirus infections in humans result from contact with infected rodents, making human-to-human transmission an exceedingly rare event globally, with the exception of the specific Andes strain implicated in the recent cruise ship incident. The primary mode of transmission involves airborne exposure to aerosolized virus particles. This occurs when fresh rodent urine, droppings, or nesting materials are disturbed, releasing tiny droplets containing the virus into the air. Individuals can then inhale these contaminated aerosols, leading to infection.
The Nevada Office of State Epidemiology (NOSE) explicitly states, “When fresh rodent urine, droppings, or nesting materials are stirred up, tiny droplets containing the virus get into the air.” Beyond inhalation, direct contact can also lead to infection. It is possible to contract hantavirus if one touches surfaces or objects contaminated with rodent excretions and then touches their nose or mouth before proper handwashing. Furthermore, scientists have posited that consuming food contaminated by the urine, droppings, or saliva of an infected rodent could also lead to illness, although this pathway is less commonly documented. A concerning aspect of hantavirus transmission is that approximately one-third of infected patients report never having seen any rodents, highlighting that even subtle signs of infestation warrant caution. Symptoms of HPS typically manifest one to eight weeks after exposure, making it challenging to pinpoint the exact moment of contact.
In the Western United States, particularly in states like Colorado and Nevada, the deer mouse (Peromyscus maniculatus) is the primary carrier responsible for human infections. This species thrives in woodland habitats, making outdoor environments a significant risk area. Studies indicate that roughly 15% of deer mice are carriers of the hantavirus, and among those exposed to infected mice, transmission rates can be as high as 40%. This ecological link underscores why individuals who frequently engage in outdoor activities, especially those involving prolonged stays in cabins, shelters, or backcountry huts, face a higher occupational or recreational risk compared to the general population.
Geographic Prevalence and Historical Data in the U.S.
While the recent cruise ship event brought hantavirus into the spotlight for a broader audience, the disease has a well-documented history in the United States, particularly in the western regions. From 1993 to 2023, the CDC recorded 890 cases of hantavirus in the U.S., with a consistent fatality rate of around 35%. A staggering 94% of these cases originated west of the Mississippi River, firmly establishing the American West as the primary endemic zone for Hantavirus Pulmonary Syndrome.
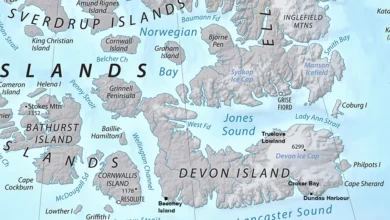
New Mexico and Colorado lead the nation in reported infections, with 129 and 121 cases, respectively. These states, characterized by expansive natural landscapes and significant deer mouse populations, present a higher environmental risk. Certain localized areas within these states and others also exhibit elevated case numbers. For instance, Mono County in California, known for its large rodent population, has recorded 27 cases, the highest in the state. Tragically, in April 2025, local authorities in Mono County reported three hantavirus-related deaths in the town of Mammoth Lakes, serving as a stark reminder of the ongoing threat to residents and visitors in these high-risk regions.
History of hantavirus in Colorado. Graph: Colorado Department of Public Health & Environment

The localized nature of outbreaks and the clear geographical distribution highlight the importance of regional public health initiatives focused on rodent control and public education. These efforts are crucial for informing residents and tourists about the risks and preventive measures tailored to specific environments where hantavirus is more prevalent.
Risk Factors and Comprehensive Prevention Strategies
Beyond the recent cruise ship anomaly, several occupations, living situations, and recreational activities significantly increase an individual’s potential contact with rodents and, consequently, their risk of contracting hantavirus. Professions such as construction workers, pest control technicians, and utility workers, who frequently encounter enclosed spaces like crawl spaces, attics, and abandoned buildings, are at elevated risk. However, it’s not just professional exposure; Washington State University notes that the majority of exposures (70%) occur "around the home." This statistic underscores the pervasive nature of the threat and its relevance to everyday life, not just remote wilderness excursions.
For outdoor enthusiasts, particularly backpackers and campers, the risk is particularly pertinent. Sleeping in cabins, remote shelters, or backcountry huts—environments often shared with mice—means potential exposure to these disease-carrying rodents. The Nevada epidemiology office clearly states, "The chance of being exposed to hantavirus is greatest when people work, play, or live in closed spaces where rodents are actively living."
To effectively reduce the chances of infection, a multi-faceted approach to prevention is essential:
1. Inspect and Avoid Rodent-Infested Areas:
- Before occupying any cabin, shelter, or hut, thoroughly examine the premises for signs of rodent activity. Look for droppings, nesting materials (shredded paper, fabric), gnaw marks on walls or food containers, and listen for scratching noises. A musty odor can also indicate a rodent presence.
- If clear evidence of rodent infestation is found, it is safest to find alternative accommodation. If staying is unavoidable, proceed with extreme caution and implement rigorous cleaning protocols.
2. Safe Food Storage and Handling:
- Always store food in rodent-proof containers, such as hard-sided plastic bins or metal canisters, both at home and in the backcountry.
- Never leave food uncovered or accessible to rodents.
- When preparing and consuming food outdoors, ensure hands are clean and surfaces are disinfected.
3. Maintain Gear and Shelter Integrity:

- For campers, ensure tents are in good repair, free of holes or gaps that rodents could exploit.
- Keep tent zippers closed and secure.
- Store backpacks and other gear inside the tent or in rodent-proof containers.
4. Proper Cleaning of Contaminated Areas:
- If rodent droppings or nesting materials are discovered, never sweep or vacuum them dry, as this can aerosolize the virus.
- Instead, wear gloves and a respirator (N95 or higher) and thoroughly wet down the area with a disinfectant solution (e.g., a bleach solution of 1 part bleach to 10 parts water) or a commercial disinfectant.
- Allow the disinfectant to sit for at least 5-10 minutes before wiping up the materials with paper towels.
- Double-bag and dispose of all contaminated materials and cleaning supplies in a sealed outdoor trash receptacle.
- Mop or sponge the entire area with disinfectant.
- After cleaning, wash hands thoroughly with soap and water.
This drawer shows some tell-tale signs of rodent infestation. Photo: CDC, Public Health Image Library
5. General Rodent Control at Home and Work:
- Seal up holes and gaps in homes and buildings to prevent rodent entry.
- Trap rodents using snap traps; avoid live traps which can release infected animals.
- Keep areas around the home clean and free of clutter that could serve as rodent habitats.
- Store pet food in sealed containers and clean up spills promptly.
Not Contagious Between Humans (with a Crucial Exception)
A critical piece of information for public understanding is that, typically, hantavirus is not contagious from one human to another. The vast majority of global cases stem directly from human contact with infected rodent excretions. However, the recent cruise ship outbreak involving the rare Andes strain serves as a stark reminder of exceptions to this rule. This particular variant has demonstrated person-to-person transmissibility, which is why the 17 American passengers were subject to such stringent quarantine and monitoring protocols.
Public health officials consistently advise treating any rodent sighting as a potential hantavirus exposure, regardless of the perceived species. Colorado’s Department of Public Health & Environment states, "All rodent exposures should be considered as potential hantavirus exposures since deer mice may be present in the same environments as house mice, even if they aren’t seen." This underscores the need for universal precautions when dealing with rodent infestations.
If personal gear or clothing has been exposed to or touched by rodents, careful handling is paramount. Individuals should wear a mask (N95 respirator) and gloves to handle the items. Contaminated items should then be disinfected using appropriate solutions or washed in hot water with detergent.
The public reaction to the cruise ship incident, marked by the surge in online searches, reflects a natural concern when a rare and deadly disease suddenly appears in an unexpected context. However, it is essential for the public to differentiate between the exceptional circumstances of the cruise ship outbreak and the more common, geographically specific risks associated with hantavirus. For the majority of people, particularly those in urban or suburban environments with good sanitation, the risk remains extremely low. The primary message for prevention continues to be diligent rodent control in and around homes and adherence to safety protocols for those who recreate or work in environments where rodents, especially deer mice, are prevalent. Public health agencies, including the CDC and state epidemiology offices, remain vigilant in monitoring cases and providing updated guidance to ensure public safety and mitigate the spread of this serious, albeit rare, disease.